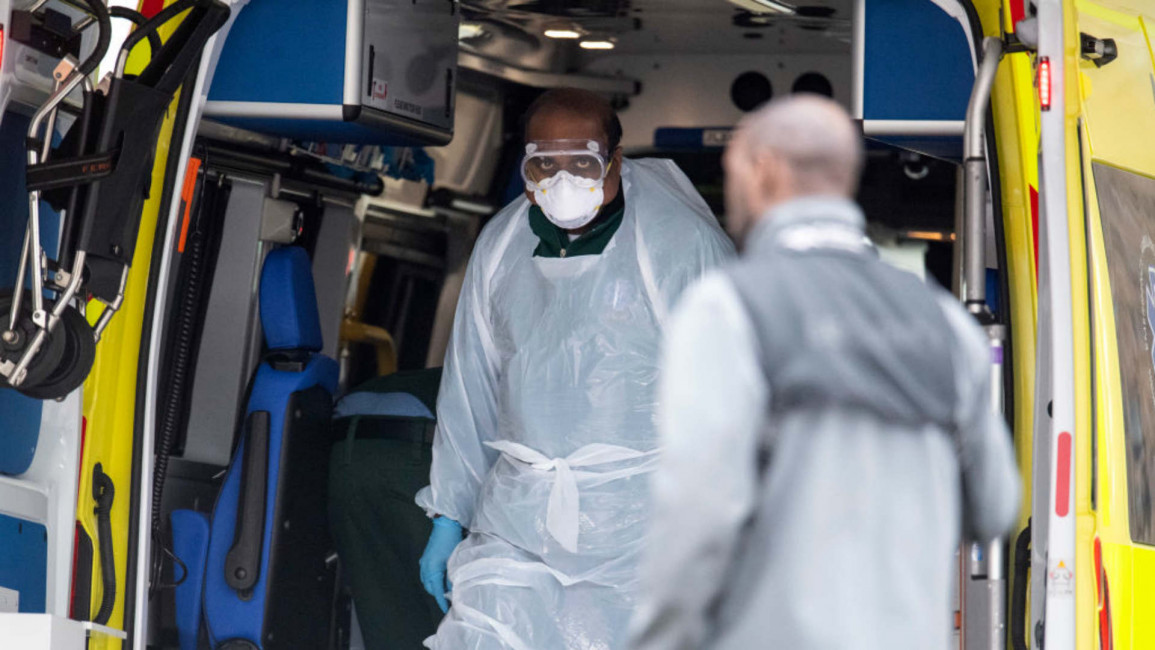
Coronavirus is killing NHS workers. Their deaths were preventable
The coronavirus has gripped British society in a vice of fear. Officially, the current death toll stands at 5,373, although it was recently revealed that deaths that had occurred outside hospitals were not being factored into the final numbers.
Figures compiled by the Office of National Statistics are drawn from death certificates, and do include those who have died at home or in care homes. In fact, these missing deaths are believed to represent a 24 percent increase in the death toll overall, suggesting that one in five deaths from coronavirus takes place outside of hospital.
The government, having spent the last decade dedicated to an NHS policy of death by a thousand cuts, is now disingenuously encouraging people to clap for the very institution they attempted to run into the ground.
The 750,000 applicants to volunteer in the NHS have been much vaunted by the PM and others, but the question is, what kind of danger will they be in?
The World Health Organization early on emphasised the importance of widespread testing, the effectiveness of which has been clearly demonstrated in South Korea and Singapore. Despite finally procuring some sort of testing facilities, we now know that less than 1 percent of NHS frontline staff have been tested.
The World Health Organization also clearly recommends several items of personal protective equipment for healthcare workers dealing with coronavirus patients, such as goggles and face shields, which the British government completely ignored until only very recently.
 |
Less than 1 percent of NHS frontline staff have been tested |  |
We know that the severe shortage of Personal Protective Equipment (PPE) in the NHS is exposing its staff to an increased likelihood of infection. There are furious battles raging within the institution over the issue, with reports that staff are being muzzled from voicing concerns about this scarcity.
The Doctors' Association UK has compiled a dossier of examples where NHS staff have been threatened with disciplinary action by management for daring to publicise the lack of PPE on social media.
The British Medical Association has stated clearly that a lack of proper protection for NHS staff would have fatal consequences, and with at least seven NHS workers passing away in the last week or so, they seem to be right.
Something particularly worthy of attention, is the identity of those who died. The NHS is the largest employer of Black and Minority Ethnic people in the UK, and a majority of the victims so far are from migrant backgrounds.
Twitter Post
|
Dr Habib Zaidi, 76, believed to have migrated from Pakistan, died on 25 March. Despite having suffered "textbook symptoms" he was only admitted to hospital the night before his passing. It was eventually confirmed on 1 April that he had been suffering from the coronavirus, though it is not known whether he had been tested while still alive.
Read more: British Muslim nurse Areema Nasreen becomes UK's youngest health worker to die of coronavirus
Dr Adil el-Tayar, 63, from Sudan also died on 25 March. He had volunteered to work in the emergency department of Hereford County Hospital. His family are convinced he contracted the virus in his voluntary role. His son Osman directly pointed to a lack of PPE, wondering "If he had proper protection perhaps this wouldn't have happened." His daughter, Abeer, echoed this sentiment. "I am angry. I feel he was cheated a couple more years out of his life."
Dr Amged El-Hawrani, 55, also originally from Sudan, died on 28 March. Following several weeks battling the illness, he passed away in Leicester at Glenfield Hospital, despite being the third doctor to die suffering from the virus, he was widely reported to be the first. Perhaps he was the only one of the three to have been tested for the virus at that point. The Doctors' Association UK released a statement lamenting his death, and branding the fact many doctors have been left without PPE as "unacceptable".
Healthcare assistant and father of seven, Thomas Harvey died from cardiac arrest at home on the 27 March, aged 57. Following a period of suffering from what his family believe to be coronavirus, he collapsed in the bathroom blocking the door. His family members were forced to break down the door in order to reach him.
Harvey's daughter Tamira commented she felt he had been "let down in so many ways", and that "if he had the right equipment we wouldn't be in this predicament." Both Tamira and his son Thomas Junior identified the lack of PPE as the likely cause of his infection. His son continued that this tragedy could have been "prevented so easily if he had been diagnosed quicker."
 |
To send NHS staff, and now hundreds of thousands of volunteers into work without proper protection amounts to lethal negligence |  |
Dr Alfa Sa'adu, 68, died on 31 March. He moved to England from Nigeria at the age of 12 and spent decades of his life serving in the NHS. He eventually retired in 2017, but continued working part-time in Hertfordshire. "I remember a few weeks ago when Boris Johnson said 'be prepared to lose loved ones.' I got really angry and remember thinking 'why is he saying this? It is not the kind of thing you say on TV.' Now I understand what he means", said his son.
Nurse Aimee O'Rourke, 38, died on 1 April. She had been caring for patients in Margate when she is believed to have contracted the virus. She was a mother of three and her daughter Megan Murphy described her as "an angel" who would wear her "NHS crown forever".
At the time of the second Clap for Carers on Thursday night, Megan encouraged people to shout her mother's name in order to give her strength in her struggle for life. Unfortunately it was later that night that Aimee succumbed to the virus.
Twitter Post
|
Nurse Areema Nasreen, 36, was a British Pakistani mother of three who died on 2 April in the same hospital she had worked at for 16 years in Walsall, West Midlands. She had worked as a cleaner there for over a decade before studying nursing and graduating last year. In addition to these victims, it is likely that more NHS staff will die in the coming months.
In fact, Director of the Royal College of Nursing in Scotland, Theresa Fyffe, has said it is inevitable.
To send NHS staff, and now hundreds of thousands of volunteers into work without proper protection amounts to lethal negligence.
The Doctors' Association UK has asserted that members of staff have had to resort to buying their own PPE, and even requested donations from schools and the general public. Workers have been forced to innovate original ways of protecting themselves in these dangerous conditions. Some NHS staff have reportedly uploaded pictures to social media with improvised protective equipment fashioned out of bin bags and other materials.
Dr Amar Ahmed of Wilmslow Health Centre in Cheshire has launched a campaign requesting help from patients with finding PPE, and in Devon one patient has used a 3D printer to manufacture masks for a local doctor's surgery.
At Kings College Hospital in London, Dr Lamis Latif has set up a campaign requesting direct support from individual companies in providing PPE to all key workers, using the hashtag #AnythingIsBetterThanNothing.
All of these heroic examples are massively inspiring but they should not have to exist in the first place.
When historicised, the death toll of this pandemic will not be viewed outside the context of the necropolitical austerity which preceded it.
As the New Economics Foundation makes clear, it is impossible to "rebuild a safety net in a week after destroying it for a decade." The wounds of the dead are speaking to us loudly, but are we listening?
Since the time of writing, more NHS staff are believed to have passed away due to coronavirus. Their names are John Algos, Glen Corbin, Liz Glanister and Lynsay Coventry.
Lowkey is a hip hop artist and political campaigner who has performed everywhere from the Royal Albert Hall to the Oxford Union. He is a patron of the Palestine Solidarity Campaign, the Campaign for Nuclear Disarmament, Stop The War Coalition and the Racial Justice Network.
Follow him on Twitter: @Lowkey0nline
Opinions expressed in this article remain those of the author and do not necessarily represent those of The New Arab, its editorial board or staff.